[ad_1]
BISMARCK — Rachel Booth and her husband have tried without success for the past three years to have children.
Like many couples in that situation, the Booths have turned to fertility treatment. They’ve been through two in vitro fertilization treatment cycles. Both failed.
Booth and her husband have exhausted the $20,000 their health insurance provides for fertility treatment. The Fargo couple — she works as a high school teacher and her husband is a police officer — can’t afford the expensive treatment themselves.
Booth testified in support of a bill that would mandate coverage for fertility treatment as well as fertility preservation for cancer patients under the North Dakota Public Employees Retirement System, or PERS. Nearly 60,000 current and retired public employees and their dependents are insured through PERS.
In North Dakota, before new coverage is mandated for private insurance, it first must be tested through insurance for public employees, so passage could be a step toward a fertility treatment mandate for private health coverage.
would require coverage for fertility health care, including diagnosis and treatment. The bill had a hearing and first reading before the House Industry, Business and Labor Committee on Tuesday, Jan. 10.
“I would like to point out that I am not the only person to be facing this disease. In fact, there are many men and women that battle infertility,” Booth told the committee, citing surveys indicating that one in eight North Dakota couples struggled with infertility.
“The mental health impact and the damage it can do to a marriage is serious and disconcerting,” she said.
Tara Brandner, a nurse practitioner in Bismarck and advocate for covering fertility treatment and preservation, said there’s a perception that the treatment always involves costly in vitro fertilization, or IVF.
“It’s not always IVF,” she said. Brandner went through IVF treatment and in her practice cares for women who struggle with infertility.
In fact, she said, less than 3% of infertility cases require the treatments, while 97% can be treated with medication, lab work, ultrasound or minimally invasive interventions.
For those who require IVF treatments, however, one round can exhaust the $15,000 or $20,000 limit many insurance policies impose, Brandner said. And as Booth’s example shows, couples sometimes must undergo multiple rounds.
The bill doesn’t impose a dollar limit on fertility treatment but caps the number of covered treatments.
The bill would require coverage for three completed cycles of intrauterine insemination. Coverage also would be required for a maximum of four egg retrievals with unlimited fresh or frozen embryo transfers. The bill also mandates coverage for medical and laboratory services that reduce excess embryo creation through egg cryopreservation and thawing “in accordance with a covered individual’s religious or ethical beliefs.”
A lobbyist for the Sanford Health Plan testified in opposition to the bill and was the only person to submit written testimony against the proposal.
“We have concerns with the broad scope of the bill in terms of likely financial impact to premium,” said Dylan Wheeler, head of government affairs for the Sanford Health Plan.
Because of the broad nature of the bill, he said, “it is difficult to estimate the exact impact at this time.”
The fiscal note attached to the bill estimates the per-biennium cost to the NDPERS insurance program at
$13.6 million, or 2.1% of premium
.
Estimates of the premium cost of the fertility treatment coverage mandate range from $1.98 per member per month to $24.85, while the consultant priced the benefit at $2.38 per member per month, Wheeler said.
The national average premium cost for infertility treatment is $1.39 per member per month, and states with $100,000 lifetime maximums have shown an average cost of $1.29 per member per month, according to Brandner.
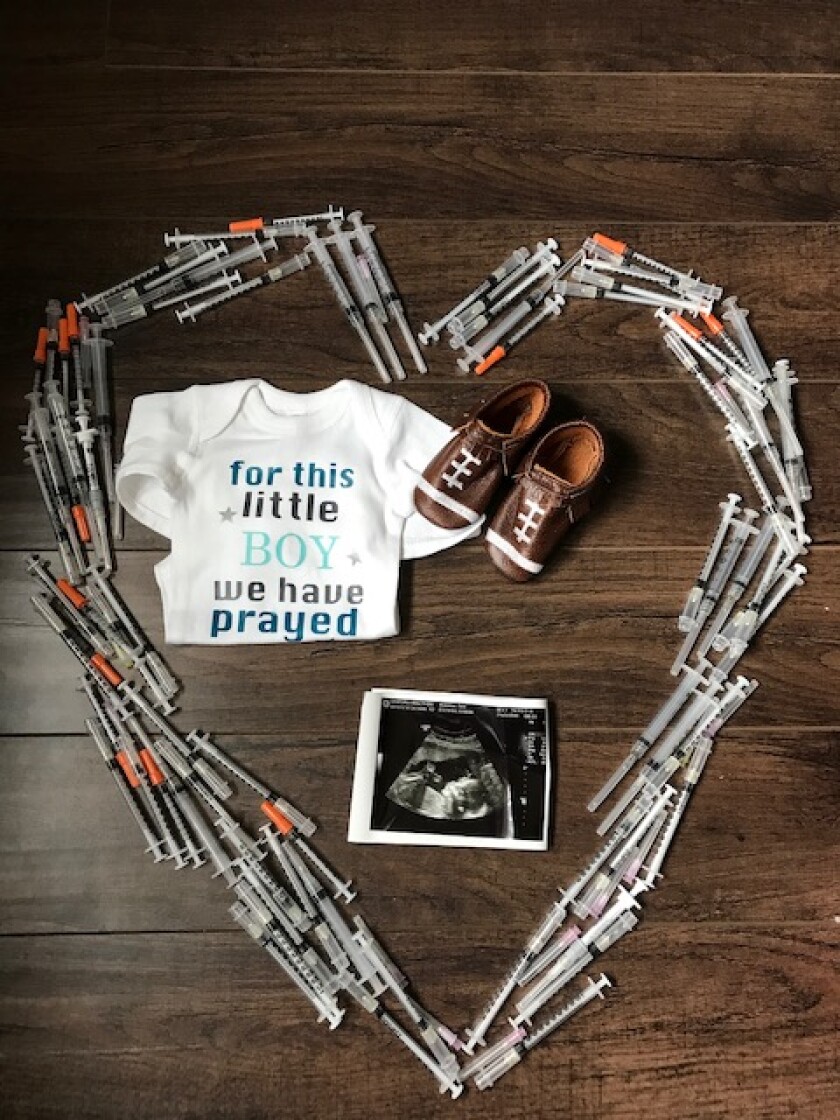
Brandner’s personal experience with fertility treatment prompted her to become an advocate for insurance coverage to help couples who are struggling to conceive.
“It’s quite the ordeal,” she said. “I wanted to do something about it.”
Patty Hulm, of Mandan, a mental health counselor and infertility support group leader, testified in support of the bill. She said she has received fertility treatment.
“I have worked with couples and individuals over the years who are facing the emotional and physical struggles of infertility all across the state of North Dakota, thanks to telehealth options and virtual meeting platforms,” she said.
“The financial barrier that couples face to build their families puts a significant strain on their relationships. It is no fault of their own that they are facing these medical conditions, but they are penalized by the lack of insurance coverage they receive because of their diagnosis of infertility,” Hulm said.
Although the emotional struggles would remain, the burden for couples would be eased knowing that portions of the expensive treatments will be covered, she said.
[ad_2]
Source link